Esther Park is a virtual patient in the Shadow Health digital clinical experience presenting with chief complaints of abdominal pain and difficulty with bowel movements. Her case involves performing a focused abdominal exam due to suspected constipation. Preparation and the correct order of abdominal assessment will be discussed in this clinical essay to help nursing students during the Shadow Health Simulation test.
Preparation.
Introduce yourself to the patient and confirm the patient’s identity. Position the patient in a supine manner and ask for the area of pain before touching. For instance, Esther Park reports lower abdominal discomfort worsened by movement.
Abdominal Assessment Steps to Follow.
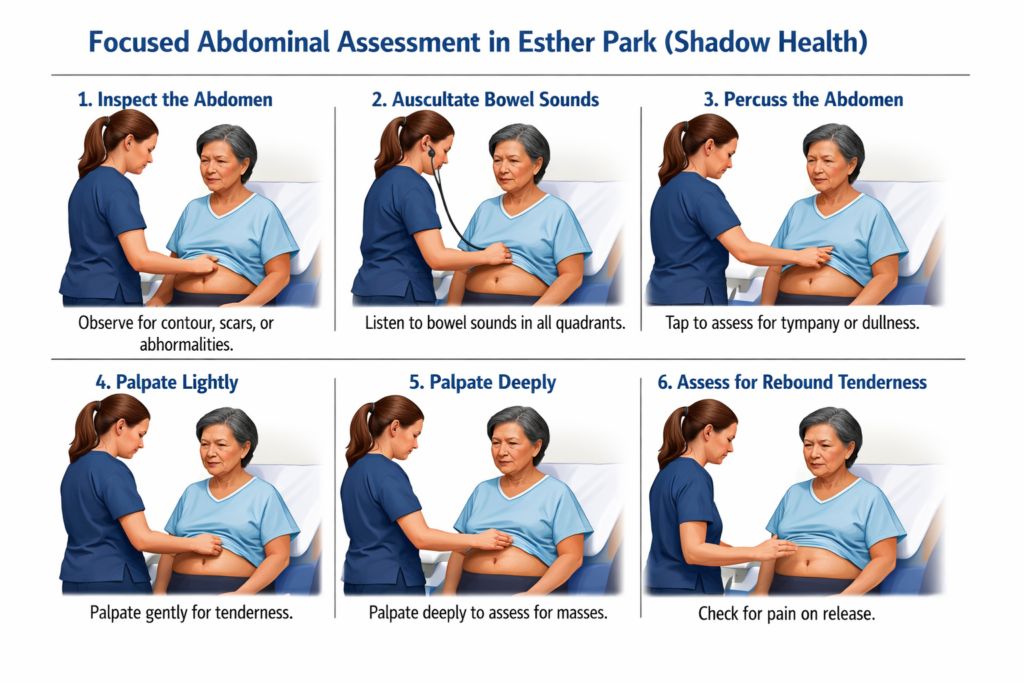
- Inspection: Observe the skin around the abdomen and inspect for contour and symmetry, visible masses and the umbilicus. For instance, Esther’s case presented findings as “Abdomen slightly distended, symmetric, no visible abnormalities beyond mild bloating.” which is common in patients who are constipating caused by fecal retention.
- Auscultation: Using the diaphragm of the stethoscope, listen in all the four quadrants (RLQ, RUQ, LUQ, LLQ) starting with the RLQ. Assess for bowel sounds (this includes frequency, pitch and character) and listen for vascular sounds. For instance, Esther’s findings presented ”Norma-active bowel sounds in all four quadrants. No bruits or friction rubs.” This rules out obstruction or hypo-active sounds but is consistent with constipation.
- Percussion: Percuss the abdomen lightly in all the four quadrants for sounds. Also, assess for organ borders if needed. For instance, Esther’s findings present the following characteristics ”Tympanic throughout most quadrants, but scattered dullness in the LLQ. No shifting dullness.”This suggests retained feces in the colon, a key clue for constipation.
- Palpation: Perform light palpation first ( to watch for tenderness, guarding or masses) before deep palpation (to assess organs/masses.)Note any special signs if observed. For instance, Esther’s case presented findings as follows;
- Light palpation: Tenderness in lower quadrants, especially LLQ; patient verbalizes pain and shows guarding.
- Deep Palpation: Palpable oblong mass in LLQ (consistent with fecal loading.)
After following the assessment procedure above, document your findings in order to help the nursing student come up with a care plan for the patient at the tail end.
Conclusion.
Based on Esther Park’s simulation, the nursing student is able to synthesize subjective data collected with the objective data observed to come up with the best care plan for the patient hence enhancing clinical reasoning needed during real-life patient interactions.