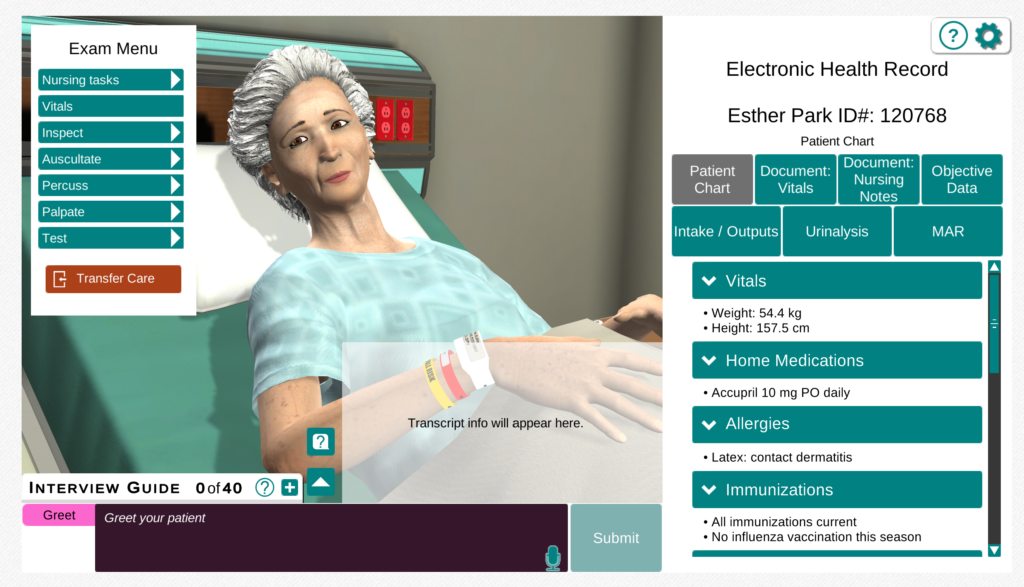
Shadow Health has transformed nursing simulation through offering very realistic hands-on experiences and interactive to bridge the gap between theory and practice. This case study focuses on Esther Park, a 78-year-old Korean American woman. The Shadow Health simulation illustrates how the platform provides nursing students with the much-needed skills in the management of chronic conditions.
Esther shows up to the clinic complaining of abdominal pains and bowel movement difficulties, and this situation helps to emphasize the difficulties that gastrointestinal examination poses when working with geriatric patients. This practical experience is where the students get to think clinically by gathering full information, diagnosing the underlying problems such as constipation, and developing holistic care strategies that concern long-term health care.
According to Esther Park, her abdominal pain developed around five days ago when she felt some general discomfort, which was accompanied by the growing difficulty in passing stool. She reports the pain started out as crampy and dull, but it has been worse over the last two to three days. The pain is mainly in the lower abdomen with a general uneasiness all through. She reports difficulty in defecating, stool deficiency (less than two a week), and absence of bowel movement within the last five days.
Esther denies recent diarrhea other than a case of food poisoning six months ago and denies nausea, vomiting, blood in stool, and any notable changes in appetite other than a slight reduction on the basis of discomfort. The visit was requested by her daughter, who believes that Esther does not look like her usual self, has been spending more time in bed on the couch, and appears exhausted. This presentation highlights major geriatric issues, as patients can reduce symptoms or delay the appointment, and it is important to conduct a detailed, communicative interview based on cultural and age considerations.
One of the most important points about the case is an inquiry into the medical history of Esther when the diagnosis is chronic hypertension treated with Accupril. She takes the medication regularly and follows up after every breakfast but complains about taking any further pharmaceuticals because of the side effects, like stomach irritation from over-the-counter drugs. Esther is traditional in her diet, and it is usually low in fiber, as people prefer soft food, and she reports a lack of physical exercise, which also leads to her symptoms.
Questions concerning psychosocial factors, food intake, toilet behavior, recent travels, vaccinations, and family support indicate how self-management of chronic disease intersects with lifestyle. Nurses get to learn about questioning sensitively to uncover obstacles such as cultural dietary practices or medication beliefs with the aim of promoting the concept of clinical thinking in the determination of risk factors that can be modified to complications.
In Shadow Health, the objective gastrointestinal examination is based on the subjective data with a systematic physical examination. The vital signs are usually stable blood pressure (indicating managed hypertension), normal temperature, and no evidence of acute distress other than mild fatigue. Examination shows a flat abdomen, without any discoloration, scars, or palpable pulsations. Auscultation provides normoactive bowel sounds on all quadrants, but no bruits or friction rubs.
Percussion has shown dominant tympany, and there is scattered dullness in the left lower quadrant (LLQ), which is indicative of a mass. Light and deep pressing of the lower abdomen, particularly the LLQ, will reveal pain, mild guarding, and an oblong mass that can be felt that is indicative of fecal impaction. Other physical examinations, including wet mucous membranes and normal skin turgor, eliminate severe dehydration, whereas a normal urinalysis eliminates the involvement of the urinary tract. Nurses who are trained on these results learn how to differentiate between benign chronic problems and emergencies and strengthen pattern recognition in older adults with multiple comorbidities.
Clinical reasoning is a combination of findings that prioritize diagnosis. The symptoms of Esther, such as constipation, abdominal pains, distension, palpable mass, and fatigue, are strong indications of constipation due to lack of adequate fiber, poor mobility, potential effects of medication, and slow bowel movements as a result of age. Her condition is exacerbated by her chronic hypertension since bad bowel habits can slow down activity and bring about discomfort, which can indirectly have an impact on blood pressure management.
The absence of red flags requires the students to exclude the possibility of differentials such as bowel obstruction, diverticulitis, or malignancy. The focus on constipation is on the treatment of the core of the problem before it leads to the formation of a fecal impaction or even perforation, which is why the prevention of the disease issue is more related to changing diet and enhancing physical activity than to the need to treat a fecal impaction.
Opportunities for patient education and empathy enhance learning. The unwillingness of Esther to use laxatives or other medications stipulates the need to discuss non-pharmacologic therapy, high-fiber food, fluids, mild physical activity, and the need to use short-term interventions such as stool softeners or enemas with their possible side effects (cramping, nausea). Nurses practice describing ideas in an understandable way, taking into consideration her independence and cultural background, including using some familiar Korean foods that are high in fiber. Therapeutic communication fosters trust, which deals with her issues of downplaying of the symptoms and family involvement which is essential in long-term compliance in chronic care.
Professional standards are supported with documentation examples. The following sample SOAP note could feature subjective complaints of lower abdominal cramping pain (6/10), constipation for five days, hypertension on Accupril, mild distension, a tender lower abdomen with a mass, normoactive bowels, no acute distress, and an assessment of constipation as an etiologic factor in acute pain in a chronic hypertension plan of adding fiber, hydration, short-term laxatives as needed, blood pressure measurements, and follow-up. Such a set format sharpens accuracy as well as prepares electronic health records.
Finally, the Esther Park-specific test about the abdominal pain in Shadow Health is a masterpiece in educating patients on the management of chronic diseases, as it simulates the interaction between acute symptoms and chronic diseases. The learners sharpen their skills in gastrointestinal assessment, improve clinical reasoning by synthesizing data, learn empathetic education, and generate comprehensive documentation, which are essential in the treatment of older adults with multimorbidity. Knowledge of this case will enable future nurses to advance self-management, avoid complications, and provide patient-centered care to their clients in practice.
For more articles you can get them in our website at Taic Research using the Link:https://taicresearch.com/articles/
References
Centers for Disease Control and Prevention. (n.d.). CDC. https://www.cdc.gov/
MedlinePlus. (n.d.). MedlinePlus – Health Information from the National Library of Medicine. https://medlineplus.gov/
NANDA International, Inc. (2025, October 14). NANDA International, Inc | Home. NANDA International, Inc |. https://www.nanda.org/ Shadow Health Health Assessment Digital Clinical ExperiencesTM for undergraduate nursing students. (n.d.). www.elsevier.com. https://www.elsevier.com/products/shadow-health/health-assessment